Dear whoever is interested,
Dear whoever is interested,
I am currently enrolled in Health Care Management, a Master’s course taught at McGill University. Some of you have shown an interest in the subject as well as voiced very interesting and provocative questions and ideas.
In response to that interest, and to aid in my own learning, I am going to make weekly(ish) posts with summaries of what was discussed in the class the previous week.
If you are at all interested in reading or commenting please do so. Discussions are where learning really happens, and where ideas are formed. It will also give us the opportunity to share some field-specific data and perhaps formulate changes that could help improve the system for all of us.
Thank you for your interest. I hope to chat with you soon.
-Jacenta
Health Care Management
Summary – Week 1
January 5th, 2011
In health care management there are five key economic principles that come into play:
- Costs
There is no limit to how much money we can throw at health care. Increases in health care spending could continue until immortality is achieved for every citizen. - Outcomes
There need to be results (presumably benefits) of the health care system. - Effectiveness
The relationship between Costs and Outcomes is of the utmost importance. Only when a treatment/idea proves adequately effective should it be funded through health care. Take, for example, the cancer drug Avastin. Canada may refuse to offer this (extremely expensive) drug to cancer patients because it seems that in the end it only lengthens lives by two weeks. (Note: This is an average. For some, it may be longer. If there was a clear determining factor for its success it could be used more discerningly, thus increasing its effectiveness.) - Trade Offs
With a fixed budget, health care is a constant juggling act. When we give more money to pharmaceuticals we must take money from somewhere else. On an even grander scale, if we want more money for health care do we take it from education? transportation? security? Or just increase taxes? - Structure
Health care can also be manipulated through its structure. Using non-monetary incentives and organization techniques the system may be altered and potentially improved.
______________________________________
Now let’s talk about Health: What makes a healthy society?
An initial reaction is often to say Access to Health Care. Interestingly, this only accounts for 25% of health. Biology accounts for another 15% (including things like gender and genetics). And Physical Environment covers 10% (including clean air and water, food and shelter).
The most influential determinant of health at a whopping 50% is Social and Economic Environment. Topping this list is socio-economic status (i.e. how much money you make), but also important are your social support netoworks (e.g. do your friends keep you physically active? do they smoke or drink? do they engage your mind?).
Clearly these categories are not mutually exclusive. For example, your socio-economic status will often dictate what physical environment you live in and therefore the quality of your air, food, water and shelter.
Also note that this is only one of the percentage-per-category correlations. Other researchers present the data differently. For example, a chart produced by the Georgia Health Policy Centre uses data from the McGinnis and Foege publication “Actual Causes of Death in the United States” (Journal of the American Medical Association, 1993). This chart rates the determinants of health as:
51% – Lifestyle (smoking, obesity, stress, nutrition, blood pressure, alcohol, drug use)
20% – Human Biology
19% – Environment
10% – Health Care
Note: The research article used to support the above percentages only provides data for the Lifestyle section (~50%). It is unclear how they calculated the other sections. Also note that the original article states that Sexual Choices are a high ranking Lifestyle factor.
To hammer home the idea of social factors playing such a crucial role in health, take a look at this video: Judy Heyman Public Health (highly recommended).
______________________________________
To Truly have Health Care in Canada, we need Canadians to care about health.
Let’s start with food.

(Image from Greek Reporter)
In 2008 the British Medical Journal published a meta-analysis of the Mediterranean Diet. The Mediterranean Diet which focuses on whole grains and fresh fruit and vegetables has an astonishing impact on longevity and health. In fact, adherence to the Mediterranean Diet has “been found to be associated with a reduction of overall mortality and mortality from cardiovascular diseases and cancer” (2008, pg. 1).
To completely convince you, take a look at these (from the 2008 article):
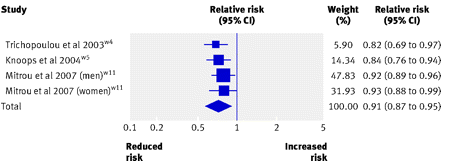
Figure 1:
Risk of all cause mortality associated with two point increase in adherence score for Mediterranean diet. Squares represent effect size; extended lines show 95% confidence intervals; diamond represents total effect size.
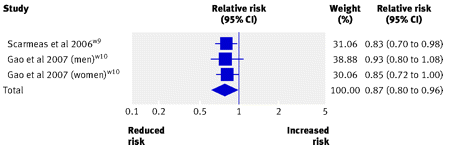
Figure 2:
Risk of Parkinson’s disease and Alzheimer’s disease associated with two point increase in adherence score for Mediterranean diet. Squares represent effect size; extended lines show 95% confidence intervals; diamond represents total effect size.
A Health Care System alone does not ensure health. As we see in the numbers, without the other systems we support as a society (such as nutrition and lifestyle as part of our education system) we would have decreased health. Clearly a trade off from the education sector to the health sector would be detrimental – just like reducing the number of preventative general practitioners (GPs) in order to increase emergency room use, which we would never do…errr…more about this next week.